Abstract
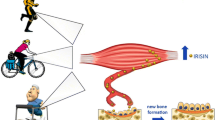
Myostatin, a member of the transforming growth factor beta (TGF-β) superfamily, was first described in 1997. Since then, myostatin has gained growing attention because of the discovery that myostatin inhibition leads to muscle mass accrual. Myostatin not only plays a key role in muscle homeostasis, but also affects fat and bone. This review will focus on the impact of myostatin and its inhibition on muscle mass/function, adipose tissue and bone density/geometry in humans. Although existing data are sparse, myostatin inhibition leads to increased lean mass and 1 study found a decrease in fat mass and increase in bone formation. In addition, myostatin levels are increased in sarcopenia, cachexia and bed rest whereas they are increased after resistance training, suggesting physiological regulatory of myostatin. Increased myostatin levels have also been found in obesity and levels decrease after weight loss from caloric restriction. Knowledge on the relationship of myostatin with bone is largely based on animal data where elevated myostatin levels lead to decreased BMD and myostatin inhibition improved BMD. In summary, myostatin appears to be a key factor in the integrated physiology of muscle, fat, and bone. It is unclear whether myostatin directly affects fat and bone, or indirectly via muscle. Whether via direct or indirect effects, myostatin inhibition appears to increase muscle and bone mass and decrease fat tissue—a combination that truly appears to be a holy grail. However, at this time, human data for both efficacy and safety are extremely limited. Moreover, whether increased muscle mass also leads to improved function remains to be determined. Ultimately potential beneficial effects of myostatin inhibition will need to be determined based on hard outcomes such as falls and fractures.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
• Cruz-Jentoft AJ, Baeyens JP, Bauer JM, Boirie Y, Cederholm T, Landi F, et al. Sarcopenia: European consensus on definition and diagnosis: report of the European working group on sarcopenia in older people. Age Ageing. 2010;39(4):412–23. doi:10.1093/ageing/afq034. Article proposes a consensus definition for sarcopenia and also gives a concise overview over the sarcopenia syndrome itself.
Fielding RA, Vellas B, Evans WJ, Bhasin S, Morley JE, Newman AB, et al. Sarcopenia: an undiagnosed condition in older adults. Current consensus definition: prevalence, etiology, and consequences. International working group on sarcopenia. J Am Med Dir Assoc. 2011;12(4):249–56.
Lang T, Streeper T, Cawthon P, Baldwin K, Taaffe DR, Harris TB. Sarcopenia: etiology, clinical consequences, intervention, and assessment. Osteoporos Int. 2010;21(4):543–59. doi:10.1007/s00198-009-1059-y.
Malafarina V, Uriz-Otano F, Iniesta R, Gil-Guerrero L. Sarcopenia in the elderly: diagnosis, physiopathology and treatment. Maturitas. 2012;71(2):109–14. doi:10.1016/j.maturitas.2011.11.012.
Muscaritoli M, Anker SD, Argiles J, Aversa Z, Bauer JM, Biolo G, et al. Consensus definition of sarcopenia, cachexia and pre-cachexia: joint document elaborated by Special Interest Groups (SIG) "cachexia-anorexia in chronic wasting diseases" and "nutrition in geriatrics". Clin Nutr (Edinburgh, Scotland). 2010;29(2):154–9. doi:10.1016/j.clnu.2009.12.004.
Rolland Y, Czerwinski S, Abellan Van Kan G, Morley JE, Cesari M, Onder G, et al. Sarcopenia: its assessment, etiology, pathogenesis, consequences and future perspectives. J Nutr Health Aging. 2008;12(7):433–50.
Walston JD. Sarcopenia in older adults. Curr Opin Rheumatol. 2012;24(6):623–7. doi:10.1097/BOR.0b013e328358d59b.
Ferrucci L, Russo CR, Lauretani F, Bandinelli S, Guralnik JM. A role for sarcopenia in late-life osteoporosis. Aging Clin Exp Res. 2002;14(1):1–4.
Bijlsma AY, Meskers CG, Westendorp RG, Maier AB. Chronology of age-related disease definitions: osteoporosis and sarcopenia. Ageing Res Rev. 2012;11(2):320–4. doi:10.1016/j.arr.2012.01.001.
• Digirolamo DJ, Kiel DP, Esser KA. Bone and skeletal muscle: neighbors with close ties. J Bone Miner Res. 2013;28(7):1509–18. Article reviews the current data on muscle – bone interactions including genetics and mechanotransduction.
Sirola J, Kroger H. Similarities in acquired factors related to postmenopausal osteoporosis and sarcopenia. J Osteoporos. 2011. doi:10.4061/2011/536735.
Baumgartner RN, Wayne SJ, Waters DL, Janssen I, Gallagher D, Morley JE. Sarcopenic obesity predicts instrumental activities of daily living disability in the elderly. Obes Res. 2004;12(12):1995–2004. doi:10.1038/oby.2004.250.
Stenholm S, Harris TB, Rantanen T, Visser M, Kritchevsky SB, Ferrucci L. Sarcopenic obesity: definition, cause and consequences. Curr Opin Clin Nutr Metab Care. 2008;11(6):693–700. doi:10.1097/MCO.0b013e328312c37d00075197-200811000-00004.
Zamboni M, Mazzali G, Fantin F, Rossi A, Di Francesco V. Sarcopenic obesity: a new category of obesity in the elderly. Nutr Metab Cardiovasc Dis. 2008;18(5):388–95. doi:10.1016/j.numecd.2007.10.002.
Rosen CJ, Bouxsein ML. Mechanisms of disease: is osteoporosis the obesity of bone. Nat Clin Pract Rheumatol. 2006;2:35–43.
Zhao LJ, Liu YJ, Liu PY, Hamilton J, Recker RR, Deng HW. Relationship of obesity with osteoporosis. J Clin Endocrinol Metab. 2007;92:1640–6.
Chumlea WC, Cesari M, Evans WJ, Ferrucci L, Fielding RA, Pahor M, et al. Sarcopenia: designing phase IIB trials. J Nutr Health Aging. 2011;15(6):450–5.
van Kan Abellan G, Cameron Chumlea W, Gillette-Guyonet S, Houles M, Dupuy C, Rolland Y, et al. Clinical trials on sarcopenia: methodological issues regarding phase 3 trials. Clin Geriatr Med. 2011;27(3):471–82. doi:10.1016/j.cger.2011.03.010.
• Pedersen BK, Febbraio MA. Muscles, exercise and obesity: skeletal muscle as a secretory organ. Nat Rev Endocrinol. 2012;8(8):45765. doi:10.1038/nrendo.2012.49. Article describes various “myokines” including myostatin and their potential effects on the human body.
McPherron AC, Lawler AM, Lee SJ. Regulation of skeletal muscle mass in mice by a new TGF-beta superfamily member. Nature. 1997;387(6628):83–90. doi:10.1038/387083a0.
McPherron AC, Lee SJ. Double muscling in cattle due to mutations in the myostatin gene. Proc Natl Acad Sci U S A. 1997;94(23):12457–61.
•• Allen DL, Hittel DS, McPherron AC. Expression and function of myostatin in obesity, diabetes, and exercise adaptation. Med Sci Sports Exerc. 2011;43(10):1828–35. doi:10.1249/MSS.0b013e3182178bb4. Article outlines the physiology of myostatin with particular attention to its role in obesity and diabetes.
Lee SJ. Regulation of muscle mass by myostatin. Annu Rev Cell Dev Biol. 2004;20:61–86. doi:10.1146/annurev.cellbio.20.012103.135836.
•• Elliott B, Renshaw D, Getting S, Mackenzie R. The central role of myostatin in skeletal muscle and whole body homeostasis. Acta Physiol (Oxf). 2012;205(3):324–40. doi:10.1111/j.1748-1716.2012.02423.x. Article gives a great overview over the history of myostatin from its discovery to signaling mechanisms to available animal and human data in muscle and other tissues.
Argiles JM, Orpi M, Busquets S, Lopez-Soriano FJ. Myostatin: more than just a regulator of muscle mass. Drug Discov Today. 2012;17(13–14):702–9. doi:10.1016/j.drudis.2012.02.001.
McNally EM. Powerful genes–myostatin regulation of human muscle mass. N Engl J Med. 2004;350(26):2642–4. doi:10.1056/NEJMp048124.
Huang Z, Chen X, Chen D. Myostatin: a novel insight into its role in metabolism, signal pathways, and expression regulation. Cell Signal. 2011;23(9):1441–6. doi:10.1016/j.cellsig.2011.05.003.
Gonzalez-Cadavid NF, Taylor WE, Yarasheski K, Sinha-Hikim I, Ma K, Ezzat S, et al. Organization of the human myostatin gene and expression in healthy men and HIV-infected men with muscle wasting. Proc Natl Acad Sci U S A. 1998;95(25):14938–43.
Sharma M, Langley B, Bass J, Kambadur R. Myostatin in muscle growth and repair. Exerc Sport Sci Rev. 2001;29(4):155–8.
Lee SJ, Lee YS, Zimmers TA, Soleimani A, Matzuk MM, Tsuchida K, et al. Regulation of muscle mass by follistatin and activins. Mol Endocrinol. 2010;24(10):1998–2008. doi:10.1210/me.2010-0127.
Rosenberg IH. Sarcopenia: origins and clinical relevance. J Nutr. 1997;127(5 Suppl):990S–1S.
Reardon KA, Davis J, Kapsa RM, Choong P, Byrne E. Myostatin, insulin-like growth factor-1, and leukemia inhibitory factor mRNAs are upregulated in chronic human disuse muscle atrophy. Muscle Nerve. 2001;24(7):893–9.
Zachwieja JJ, Smith SR, Sinha-Hikim I, Gonzalez-Cadavid N, Bhasin S. Plasma myostatin-immunoreactive protein is increased after prolonged bed rest with low-dose T3 administration. J Gravit Physiol. 1999;6(2):11–5.
Ju CR, Chen RC. Serum myostatin levels and skeletal muscle wasting in chronic obstructive pulmonary disease. Respir Med. 2012;106(1):102–8. doi:10.1016/j.rmed.2011.07.016.
Remels AH, Gosker HR, Langen RC, Schols AM. The mechanisms of cachexia underlying muscle dysfunction in COPD. J Appl Physiol. 2013;114(9):1253–62. doi:10.1152/japplphysiol.00790.2012.
Han DS, Chen YM, Lin SY, Chang HH, Huang TM, Chi YC, et al. Serum myostatin levels and grip strength in normal subjects and patients on maintenance haemodialysis. Clin Endocrinol (Oxf). 2011;75(6):857–63. doi:10.1111/j.1365-2265.2011.04120.x.
Yarasheski KE, Bhasin S, Sinha-Hikim I, Pak-Loduca J, Gonzalez-Cadavid NF. Serum myostatin-immunoreactive protein is increased in 60–92 year old women and men with muscle wasting. J Nutr Health Aging. 2002;6(5):343–8.
Leger B, Derave W, De Bock K, Hespel P, Russell AP. Human sarcopenia reveals an increase in SOCS-3 and myostatin and a reduced efficiency of Akt phosphorylation. Rejuvenation Res. 2008;11(1):163–75B. doi:10.1089/rej.2007.0588.
Ratkevicius A, Joyson A, Selmer I, Dhanani T, Grierson C, Tommasi AM, et al. Serum concentrations of myostatin and myostatin-interacting proteins do not differ between young and sarcopenic elderly men. J Gerontol A Biol Sci Med Sci. 2011;66(6):620–6. doi:10.1093/gerona/glr025.
Szulc P, Schoppet M, Goettsch C, Rauner M, Dschietzig T, Chapurlat R, et al. Endocrine and clinical correlates of myostatin serum concentration in men–the STRAMBO study. J Clin Endocrinol Metab. 2012;97(10):3700–8. doi:10.1210/jc.2012-1273.
Seibert MJ, Xue QL, Fried LP, Walston JD. Polymorphic variation in the human myostatin (GDF-8) gene and association with strength measures in the women's health and aging study II cohort. J Am Geriatr Soc. 2001;49(8):1093–6.
Bhatt SP, Nigam P, Misra A, Guleria R, Luthra K, Jain SK, et al. Association of the Myostatin gene with obesity, abdominal obesity and low lean body mass and in non-diabetic Asian Indians in north India. PLoS One. 2012;7(8):e40977. doi:10.1371/journal.pone.0040977.
Yue H, He JW, Zhang H, Wang C, Hu WW, Gu JM, et al. Contribution of myostatin gene polymorphisms to normal variation in lean mass, fat mass and peak BMD in Chinese male offspring. Acta Pharmacol Sin. 2012;33(5):660–7. doi:10.1038/aps.2012.12.
Garatachea N, Lucia A. Genes and the ageing muscle: a review on genetic association studies. Age (Dordr). 2013;35(1):207–33. doi:10.1007/s11357-011-9327-0.
Santiago C, Ruiz JR, Rodriguez-Romo G, Fiuza-Luces C, Yvert T, Gonzalez-Freire M, et al. The K153R polymorphism in the myostatin gene and muscle power phenotypes in young, non-athletic men. PLoS One. 2011;6(1):e16323. doi:10.1371/journal.pone.0016323.
Roth SM, Martel GF, Ferrell RE, Metter EJ, Hurley BF, Rogers MA. Myostatin gene expression is reduced in humans with heavy-resistance strength training: a brief communication. Exp Biol Med (Maywood). 2003;6(228):706–9.
Saremi A, Gharakhanloo R, Sharghi S, Gharaati MR, Larijani B, Omidfar K. Effects of oral creatine and resistance training on serum myostatin and GASP-1. Mol Cell Endocrinol. 2010;317(1–2):25–30. doi:10.1016/j.mce.2009.12.019.
Walker KS, Kambadur R, Sharma M, Smith HK. Resistance training alters plasma myostatin but not IGF-1 in healthy men. Med Sci Sports Exerc. 2004;36(5):787–93.
Konopka AR, Douglass MD, Kaminsky LA, Jemiolo B, Trappe TA, Trappe S, et al. Molecular adaptations to aerobic exercise training in skeletal muscle of older women. J Gerontol A Biol Sci Med Sci. 2010;65(11):1201–7. doi:10.1093/gerona/glq109.
Hittel DS, Axelson M, Sarna N, Shearer J, Huffman KM, Kraus WE. Myostatin decreases with aerobic exercise and associates with insulin resistance. Med Sci Sports Exerc. 2010;42(11):2023–9. doi:10.1249/MSS.0b013e3181e0b9a8.
Hulmi JJ, Ahtiainen JP, Kaasalainen T, Pollanen E, Hakkinen K, Alen M, et al. Postexercise myostatin and activin IIb mRNA levels: effects of strength training. Med Sci Sports Exerc. 2007;39(2):289–97. doi:10.1249/01.mss.0000241650.15006.6e.
Schuelke M, Wagner KR, Stolz LE, Hubner C, Riebel T, Komen W, et al. Myostatin mutation associated with gross muscle hypertrophy in a child. N Engl J Med. 2004;350(26):2682–8. doi:10.1056/NEJMoa040933.
Fedoruk MN, Rupert JL. Myostatin inhibition: a potential performance enhancement strategy? Scand J Med Sci Sports. 2008;18(2):123–31. doi:10.1111/j.1600-0838.2007.00759.x.
Krivickas LS, Walsh R, Amato AA. Single muscle fiber contractile properties in adults with muscular dystrophy treated with MYO-029. Muscle Nerve. 2009;39(1):3–9. doi:10.1002/mus.21200.
• Attie KM, Borgstein NG, Yang Y, Condon CH, Wilson DM, Pearsall AE, et al. A single ascending-dose study of muscle regulator ACE-031 in healthy volunteers. Muscle Nerve. 2013;47(3):416–23. doi:10.1002/mus.23539. Only currently available human randomized controlled trial on myostatin pathway inhibition and its effect on muscle, fat, and bone.
Borgstein NG, Barger R, Yang Y, Wilson DM, Haltom E, Attie KM, et al. A Phase 1 multiple ascending dose study to assess the pharma-codynamic effects of ACE-031, an inhibitor of negative muscle regulators, in healthy volunteers. Neuromuscul Disord. 2010;20(9–10):646. doi:10.1016/j.nmd.2010.07.160.
McPherron AC, Lee SJ. Suppression of body fat accumulation in myostatin-deficient mice. J Clin Invest. 2002;109(5):595–601. doi:10.1172/JCI13562.
Allen DL, Cleary AS, Speaker KJ, Lindsay SF, Uyenishi J, Reed JM, et al. Myostatin, activin receptor IIb, and follistatin-like-3 gene expression are altered in adipose tissue and skeletal muscle of obese mice. Am J Physiol Endocrinol Metab. 2008;294(5):E918–27. doi:10.1152/ajpendo.00798.2007.
Rebbapragada A, Benchabane H, Wrana JL, Celeste AJ, Attisano L. Myostatin signals through a transforming growth factor beta-like signaling pathway to block adipogenesis. Mol Cell Biol. 2003;23(20):7230–42.
Lyons JA, Haring JS, Biga PR. Myostatin expression, lymphocyte population, and potential cytokine production correlate with predisposition to high-fat diet induced obesity in mice. PLoS One. 2010;5(9):e12928. doi:10.1371/journal.pone.0012928.
Feldman BJ, Streeper RS, Farese Jr RV, Yamamoto KR. Myostatin modulates adipogenesis to generate adipocytes with favorable metabolic effects. Proc Natl Acad Sci U S A. 2006;103(42):15675–80. doi:10.1073/pnas.0607501103.
Guo T, Jou W, Chanturiya T, Portas J, Gavrilova O, McPherron AC. Myostatin inhibition in muscle, but not adipose tissue, decreases fat mass and improves insulin sensitivity. PLoS One. 2009;4(3):e4937. doi:10.1371/journal.pone.0004937.
Hittel DS, Berggren JR, Shearer J, Boyle K, Houmard JA. Increased secretion and expression of myostatin in skeletal muscle from extremely obese women. Diabetes. 2009;58(1):30–8. doi:10.2337/db08-0943.
Pan H, Ping XC, Zhu HJ, Gong FY, Dong CX, Li NS, et al. Association of myostatin gene polymorphisms with obesity in Chinese north Han human subjects. Gene. 2012;494(2):237–41. doi:10.1016/j.gene.2011.10.045.
Milan G, Dalla Nora E, Pilon C, Pagano C, Granzotto M, Manco M, et al. Changes in muscle myostatin expression in obese subjects after weight loss. J Clin Endocrinol Metab. 2004;89(6):2724–7. doi:10.1210/jc.2003-032047.
Park JJ, Berggren JR, Hulver MW, Houmard JA, Hoffman EP. GRB14, GPD1, and GDF8 as potential network collaborators in weight loss-induced improvements in insulin action in human skeletal muscle. Physiol Genomics. 2006;27(2):114–21. doi:10.1152/physiolgenomics.00045.2006.
Mendias CL, Bakhurin KI, Faulkner JA. Tendons of myostatin-deficient mice are small, brittle, and hypocellular. Proc Natl Acad Sci U S A. 2008;105(1):388–93. doi:10.1073/pnas.0707069105.
Elkasrawy MN, Hamrick MW. Myostatin (GDF-8) as a key factor linking muscle mass and bone structure. J Musculoskelet Neuronal Interact. 2010;10(1):56–63.
• Hamrick MW. Myostatin (GDF-8) as a therapeutic target for the prevention of osteoporotic fractures. IBMS BoneKEy. 2010;7(1):8–17. doi:10.1138/20100423. Article which reviews the potential effects of myostatin signalling and its inhibition on bone.
Hamrick MW, Samaddar T, Pennington C, McCormick J. Increased muscle mass with myostatin deficiency improves gains in bone strength with exercise. J Bone Miner Res. 2006;21(3):477–83. doi:10.1359/JBMR.051203.
Bowser M, Herberg S, Arounleut P, Shi X, Fulzele S, Hill WD, et al. Effects of the activin A-myostatin-follistatin system on aging bone and muscle progenitor cells. Exp Gerontol. 2013;48(2):290–7. doi:10.1016/j.exger.2012.11.004.
Rothney MP, Martin FP, Xia Y, Beaumont M, Davis C, Ergun D, et al. Precision of GE Lunar iDXA for the measurement of total and regional body composition in nonobese adults. J Clin Densitom. 2012;15:399–404.
Lloyd TE. Novel therapeutic approaches for inclusion body myositis. Curr Opin Rheumatol. 2010;22(6):658–64. doi:10.1097/BOR.0b013e32833f0f4a.
Malik V, Rodino-Klapac LR, Mendell JR. Emerging drugs for Duchenne muscular dystrophy. Expert Opin Emerg Drugs. 2012;17(2):261–77. doi:10.1517/14728214.2012.691965.
Breitbart A, Auger-Messier M, Molkentin JD, Heineke J. Myostatin from the heart: local and systemic actions in cardiac failure and muscle wasting. Am J Physiol Heart Circ Physiol. 2011;300(6):H1973–82. doi:10.1152/ajpheart.00200.2011.
Anker MS, von Haehling S, Springer J, Banach M, Anker SD. Highlights of the mechanistic and therapeutic cachexia and sarcopenia research 2010 to 2012 and their relevance for cardiology. Int J Cardiol. 2013;162(2):73–6. doi:10.1016/j.ijcard.2012.10.018.
Brass EP, Sietsema KE. Considerations in the development of drugs to treat sarcopenia. J Am Geriatr Soc. 2011;59(3):530–5. doi:10.1111/j.1532-5415.2010.03285.x.
Fischetto G, Bermon S. From gene engineering to gene modulation and manipulation: can we prevent or detect gene doping in sports? Sports Med. 2013. doi:10.1007/s40279-013-0075-4.
van der Gronde T, de Hon O, Haisma HJ, Pieters T. Gene doping: an overview and current implications for athletes. Br J Sports Med. 2013;47(11):670–8. doi:10.1136/bjsports-2012-091288.
Anonymous. Overweight and Obesity. Center for Disease Control. 2013. http://www.cdc.gov/obesity/data/index.html. Accessed June 23, 2013.
Holes-Lewis KA, Malcolm R, O'Neil PM. Pharmacotherapy of obesity: clinical treatments and considerations. Am J Med Sci. 2013;345(4):284–8. doi:10.1097/MAJ.0b013e31828abcfd.
Compliance with Ethics Guidelines
ᅟ
Conflict of Interest
B. Buehring is affiliated with an institution that has received a grant from Lilly. N. Binkley has received research grants from Amgen, Lilly, Merck, and Opko and is on an advisory board for Lilly and Merck.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Buehring, B., Binkley, N. Myostatin – The Holy Grail for Muscle, Bone, and Fat?. Curr Osteoporos Rep 11, 407–414 (2013). https://doi.org/10.1007/s11914-013-0160-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11914-013-0160-5