INTRODUCTION
Rheumatoid arthritis (RA) is a systemic autoimmune inflammatory disease that affects synovial joints and lead to chronic pain, bone erosions and progressive disability. Approximately 1% of the adult population in the United States has RA, and the overall world prevalence range from 0.5% to 1%, qualifying it as the most common chronic inflammatory condition[1,2]. Beyond joint disease, evidences support the hypothesis that chronic inflammation could increase cardiovascular risk: patients with RA die earlier than the general population[3], in particular, mortality risk in RA patients is 1.5 higher than general population and occurs largely as a result of higher rates of cardiovascular death[4]. A recent meta-analysis shows that standardized mortality ratio (SMR) ranges from 0.99 to 3.82 for myocardial infarction and from 1.08 to 2 for cerebrovascular diseases[5], while risk to develop peripheral arterial diseases is 2.35 in a large cohort of United States patients. Risk to develop non fatal cardiovascular and cerebrovascular diseases, that lead to significant disability care cost is also increased in RA. These diseases are strictly related to an accelerated atherosclerotic process and, although several factors contribute independently to the heightened cardiovascular risk observed in patients with RA, systemic inflammation contributes importantly[6]. Different authors suggested in fact that the higher prevalence of cardiovascular events in RA patients could be explained by other mechanisms than the classic atherosclerotic risk factors[7-10].
We briefly review the role of subclinical atherosclerosis in RA, its relationship with inflammatory process and the non-invasive methods to detect early atherosclerotic changes and to estimate risk of cardiovascular events.
INFLAMMATION AND ATHEROSCLEROSIS IN RA
Atherosclerosis and RA share a number of similarities, including T-cell and mast cell activation, production of pro-inflammatory cytokines such as tumor necrosis factor (TNF) alpha and interleukin (IL)-6, and increased expression of leukocyte adhesion molecules[11].
Patients with RA have elevated levels of the acute-phase reactant C reactive protein (CRP), a marker of inflammation associated with increased cardiovascular risk. Moreover, CRP causes endothelial dysfunction by decreasing endothelial nitric oxide synthase, a potent anti-atherogenic factor[12].
Patients with RA with elevated erythrocyte sedimentation rate (ESR) have a higher rate of cardiovascular death than those without elevated ESR. This inflammatory marker also increases linearly with increased carotid artery intima-media thickness in both patients with RA and healthy controls[6].
Immune system plays an important role in the progression and development of atherosclerotic disease and associated complications. Atherosclerosis is in fact now considered as an autoimmune disease[6,13,14]. The presence of inflammatory cells, such as macrophages and activated lymphocytes within atherosclerotic plaque, is a strong indicator of immune system involvement. Furthermore, the inflammatory burden in RA and other rheumatologic diseases increases the process of oxidation of low density lipoproteins (ox-LDL), responsible for the formation and progression of atherosclerotic plaque[15]. ox-LDL amplifies the inflammatory response through the expression of adhesion molecules by endothelial cells and through the production of pro-inflammatory cytokines (TNF alpha, IL-1, IL-6) by macrophages[13,16]. Mature dendritic cells (DC) express CCL17 that favoring T-lymphocytes recruitment; moreover the presence of modified or native LDL, induce up-regulation of co-stimulatory molecules on DCs that lead to T-lymphocyte proliferation. Modified LDL determine the formation of new antigenic epitopes which can be presented by DCs and brought to clonal expansion of LDL-specific T-lymphocytes. Indeed, about 10% of all T-lymphocytes detectable in human atherosclerotic plaques specifically recognize modified or native LDL. Of note, LDL-specific T-lymphocytes are also present in the circulation[17]. The elevated levels of pro-inflammatory cytokines can elicit a systemic inflammatory state that could lead to pro-atherogenic phenotype: cytokines, in addition to their role in regulating immune responses, mediate a number of metabolic effects that, in the short term, mediate appropriate responses to injury or infection, but on a chronic basis prove detrimental: systemic release of IL-1, IL-17, IL-6, and TNF-α, produced in synovial tissue in RA patients, promotes a number of pro-atherogenic functions of the liver, adipose tissue, skeletal muscle, and vascular endothelium, including insulin resistance, dyslipidemia, endothelial activation, and prothrombotic and antifibrinolytic effects[14]. CRP and other factors local released by leukocytes, contributes to early endothelial dysfunction and damage.
Immunological abnormalities such as auto-antibodies production may be involved in endothelial dysfunction and in the process of progression and rupture of the atherosclerotic plaque. Rheumatoid factor could be found in the atheroma as immunocomplex and is associated with impaired endothelial function and increased mortality[18].
Atherosclerotic vascular involvement and cardiac abnormalities including pericardial, myocardial, and endocardial involvement, were higher among anti citrullinated peptide antibodies (ACPA) positive RA patients[19]. Citrullinated proteins, including citrullinated fibrinogen, are present within atherosclerotic plaque, and co-localized with peptidylarginine deiminase type 4 (PAD-4). Moreover, ACPA serum levels correlates with subclinical atherosclerosis indices. These, and other observations, support the hypothesis that citrullinated epitopes within the atherosclerotic plaque may be targeted by RA-associated ACPAs, thus forming immune complexes capable of locally perpetuating plaque inflammation and progression[20].
Several studies demonstrated that endothelial dysfunction plays a central role in the pathogenesis of atherosclerosis, promotes early atherosclerotic changes and is predictive for the development of cardiovascular events[21,22]. Patients with RA have a greater prevalence of arterial atherosclerotic plaques than controls[23,24] and the presence of atherosclerotic plaques correlate with disease duration, radiological damage index and systemic inflammation[25].
Early detection of subclinical atherosclerosis in RA could be useful to prevent cardiovascular events, death and disability. Different non-invasive methods are available to detect atherosclerosis and to estimate risk of cardiovascular events. These tools include functional and morphological assessment of artery physiology.
FLOW MEDIATED DILATATION
The normal, healthy endothelium regulates vascular tone and structure and exerts anticoagulant, anti-platelet, and fibrinolitic properties. The maintenance of vascular tone is accomplished by the release of numerous dilator and constrictor substances. The major vasodilator substance released by the endothelium is nitric oxide (NO). Endothelial dysfunction occurs when NO bioavailability is reduced[10,21,22,26,27].
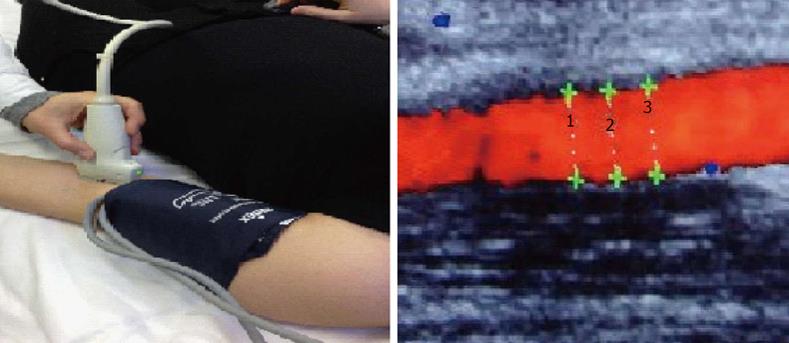
Among different methods, the assessment of flow-mediated dilatation (FMD) is one of the most used to assess the endothelial function in vivo, with a non invasive approach[28]. FMD reflects the ability of brachial artery to dilate after reactive hyperaemia induced by shear stress. It depends on the endothelial production of agents with vasomotor action, specifically NO[29-31](Figure 1).
Figure 1 Flow mediated dilatation is based on the reactive phenomenon that occurs when arterial blood flow is restored after a period of transient arterial occlusion using a sphygmomanometer.
This reactive hyperaemia is observable at ultrasound power Doppler mode monitor.
Traditional cardiovascular risk factors, such as smoking, obesity, abnormal glucose or lipid dismetabolism and hypertension, could alter endothelial function and have been related with impaired FMD. Moreover, impaired FMD predicts the risk of future cardiovascular events and it is a surrogate marker of general atherosclerosis[32-35].
Endothelial function could also be assessed with administration of sublingual nitroglycerin (NTG). NTG induces a vasodilatation that is endothelium-independent to production of local NO[36].
In RA patients, FMD is impaired, compared to controls, independent to the presence of classical atherosclerosis risk factors. RA patients showed similar FMD impairment than those with diabetes, supporting the theory that RA is an independent risk factor for atherosclerosis. Endothelial dysfunction in these patients seems to be related to disease activity (DAS28), disease duration, HLA-DRB1 shared epitope and inflammatory indices[37]. Furthermore, in RA patients disease activity, assessed by DAS28, ESR and CRP, predicts the magnitude of endothelial dysfunction[38]. FMD is impaired even in patients with early disease, suggesting that atherosclerotic process starts early[39]. Few studies demonstrate NTG-mediated vasodilatation impairment in RA patients. Hannawi et al[40] in a longitudinal study on 20 patients with early RA found that both FMD and NTG-mediated vasodilatation were significantly lower in patients in respect to control and negatively correlated with age and CRP.
INTIMA-MEDIA THICKNESS
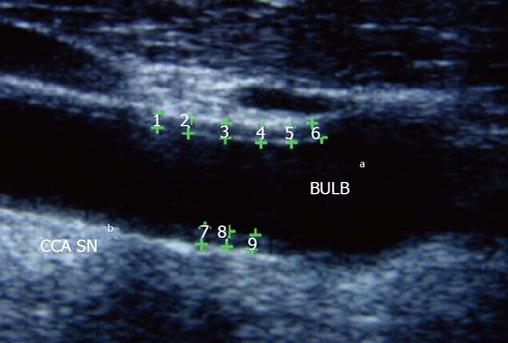
Carotid atherosclerosis may be determined by the assessment of common carotid intima-media thickness (IMT) using high-resolution B-mode ultrasound technique (Figure 2). Increased IMT is associated to the onset of cardiovascular events and is strongly related to the presence of atherosclerosis risk factors, such as hypertension, hypercholesterolemia, smoke, diabetes and obesity[41-43]. Several studies reported increased IMT in patients with rheumatic disease, in particular, patients with systemic lupus erythematosus, psoriatic arthritis and ankylosing spondylitis show increased IMT in respect to control as demonstrated in some study[44,45]. Patients with RA showed increased IMT in respect to age and sex matched controls: a meta-analysis from 22 studies, in 2011, compared carotid IMT data of 1384 RA patients with 1147 control subjects. Seventeen of 22 studies reported a statistical significant higher IMT in RA patients compared with controls. Mean IMT in RA patients was 0.71 mm and in control subjects 0.62 mm even in subject without other cardiovascular risk factors[46,47]. In RA patients IMT correlates with disease activity, severity and disease duration, with CRP, erythrocyte sedimentation rate (ESR) and use of corticosteroids[25]. Furthermore, increased IMT and carotid plaque presence predict the risk of cardiovascular morbidity in RA patients, in particular, carotid artery IMT > 0.9 has a high predictive power for the development of cardiovascular events over a 5-years period follow-up[48,49].
Figure 2 B-mode ultrasound measurement of carotid intima media thikness in patient with Rheumatoid Arthritis.
aBULB: Carotid bulb; bCCA SN: Left common carotid arteria.
ANKLE/BRACHIAL INDEX
The Ankle/Brachial Index (ABI) or Windsor’s Index represents a simple, useful, reproducible, non-invasive method to detect asymptomatic peripheral artery disease (PAD). It expresses the ratio between the systolic blood pressure in posterior tibial artery measured at the ankle, and the systolic blood pressure measured in the brachial artery. It has been used for many years to assess the severity of peripheral artery disease and to detect the presence of asymptomatic, although hemodynamically relevant, stenosis[50,51].
ABI is an indicator of generalized atherosclerosis and can provide prognostic information about cardiovascular diseases. Moreover, patients with lower values of ABI are at higher risk of myocardial infarction or stroke. In RA patients, disease activity, disease duration and corticosteroid use are risk factors for PAD. Few studies evaluated the prevalence of peripheral artery disease in patients with rheumatic disease. Del Rincòn et al[52] studied 234 patients with RA and demonstrated an increased prevalence of impaired peripheral artery function. In this study there was high percentage of peripheral artery obstruction and incompressibility in RA patients in respect to controls[52].
CORONARY CALCIUM CONTENT
Coronary atherosclerosis is the major determiner of miocardial infarction, but could be directly detectable only through invasive exams such as angiography. Indirect information about coronary atherosclerosis could be obtained by measurement of calcium content. Coronary Calcium Content (CAC) measurement is considered as surrogate marker of atherosclerosis because of its high correlation with total atherosclerotic plaques demonstrated in angiographic, hystopathologic, and ultrasound studies. CAC is a marker of subclinical atherosclerosis of the coronary district and gives quantitative measurement of the calcified share of coronary atherosclerotic plaque. Moreover, it strongly predicts the risk of cardiovascular disease in general population[53].
Recent evidences suggest that measurement of CAC is predictive of myocardial infarction and cardiovascular disease at 5 years and the use of CAC can provide important informations, independent from the other traditional cardiac risk factors[53,54]. Different cross-sectional studies investigated the role of CAC detection in RA patients. In particular Giles et al[55] showed a higher prevalence and extent of CAC in RA patients compared with controls after adjustments for the main cardiovascular risk factors. Furthermore, patients with longstanding RA have more extensive subclinical atherosclerosis assessed by CAC compared to patients of the same age as a consequence of accelerated atherosclerosis[55]. Finally, in RA patients, higher CAC is significantly associated with serum TNF-alpha and IL-6 levels. This evidence supports the role of inflammation in the promotion of atherosclerosis, and specifically of coronary calcification in RA.
CORONARY FLOW RESERVE
Coronary flow reserve (CFR) gives indirect information on the status of coronary district through the analysis of artery flow signals. Impairment of endothelial function and reduced CFR, which reflects coronary microvascular function, has been shown to be early manifestation of atherosclerosis and coronary artery disease. CFR is measured with non invasive trans-thoracic Doppler transducer used to identify patients with known or suspected cardiovascular diseases[56,57]. CFR is impaired in patients with connective tissue diseases and RA without clinical evidence of heart disease, as a result of impaired microcirculation, as demonstrated by reduced CFR in a cohort of 81 RA patients compared with healthy controls[58]. Moreover, in RA CFR correlated with disease duration and with left ventricular function[58,59].
PULSE WAVE ANALYSIS
Arterial stiffness is one of the events that occur in the natural process of aging, but it could also be related to pathological process as arteriosclerosis. Pulse Wave Analysis (PWA) is one of the most used and reproducible method to assess arterial stiffness. PWA consists of two fundamental components: pulse wave velocity (PWV) and augmentation index (AIx). PWV is an excellent indicator of arterial compliance of large vessels. Several studies demonstrated that hypertension, diabetes and smoke, reduce the compliance of artery wall. Furthermore, PWV is associated to coronary atherosclerosis and to an higher mortality. Significantly increase in PWV was observed also in inflammatory rheumatic diseases such as SLE and RA and correlates with impaired FMD and increased IMT[60-62]. Chronic and systemic inflammation could enhance arterial stiffness increasing the presence of fibroblasts cells at endothelial level, interfering with the processes that regulates arterial vasodilation and constriction. In RA patients arterial elasticity is also inversely related with inflammation indices[60]. PWA appears to be a more sensitive test of vascular dysfunction than FMD in RA and may be the preferred marker of vascular dysfunction in RA patients. Significantly increased PWV was observed in RA patients and PWV was correlated with impaired FMD and increased IMT. Instead, arterial elasticity is decreased and is inversely associated with measures of inflammation. In a recent study Provan et al[62] demonstrated the predictive value of CRP to increased arterial stiffness in 15 year follow up RA patients, confirming the role of inflammation on early atherosclerotic changes.
SERUM BIOMARKER OF SUBCLINICAL ATHEROSCLEROSIS
In addition to traditional risk factors in RA other possible biomarkers that could be associated with the development of subclinical atherosclerosis were investigated. In particular, it has been suggested that serum biomarker could be useful to assess the presence of subclinical atherosclerosis or to estimate the risk to develop cardiovascular events. The levels of ox-LDL are associated with increased cardiovascular risk and were significantly more elevated in RA patients compared to controls. Moreover serum levels of NO in patients with RA are significantly lower than in controls and, also, correlated inversely with IMT[63].
Asymmetric-dimethylarginine (ADMA) is a molecule that inhibits endothelial NO synthase (eNOS). Elevated ADMA levels are an independent risk factor for endothelial dysfunction, and they have been associated with hypertension, diabetes, hypercholesterolemia, renal failure, and atherosclerosis in both experimental models and humans. Recent evidences demonstrated that ADMA levels are increased in RA patients in respect to control and its levels decreased after therapy[64].
Apeline is a recently described peptide that is known to be produced by several cell types. It causes endothelium-dependent vasorelaxation by triggering the release of NO. Apeline serum levels are significantly lower in RA patients[64]. Other potential biomarkers of subclinical atherosclerosis are anti-oxidant substances such as beta-carotene, vitamin E, D and C. Further studies are needed to define the role of these molecules in clinical practice.
CONCLUSION
Vascular function is abnormal in RA and the atherosclerotic process seems to be accelerated: increased arterial stiffness, reduced arterial elasticity, impaired endothelial response, increased IMT and coronary calcium content are related to presence of systemic inflammation and with increased risk of cardiovascular morbidity and mortality. The management of RA patients should be in line with the European League Against Rheumatism recommendations for the management of cardiovascular risk in patients with RA[65]: these recommendations provide adequate control of arthritis and periodic evaluations of the cardiovascular risk; in particular, treatment strategy to control cardiovascular risk factors should be based on the use of statins and ACE-inhibitors or angiotensin II blockers because of their potential anti-inflammatory effects[65]. Further studies are needed to understand the impact of traditional therapies and new biologic drugs on the development of subclinical atherosclerosis and cardiovascular risk prevention. Traditional DMARDs and anti-TNF therapy could potentially decrease cardiovascular risk and improve endothelial function through the impact on inflammation. To support this hypothesis, some studies showed improvement in endothelial function, assessed by FMD and no progression of carotid IMT, in RA patients treated with adalimumab and infliximab[66,67]. Effect of B-cells depletion therapy on subclinical atherosclerosis is still debated: some study reported no effects on arterial stiffness during 6 mo therapy with rituximab, while other evidences demonstrated beneficial effects on FMD and IMT[68,69]. In conclusion, patients and physicians should be aware of the potential cardiovascular risk of rheumatoid arthritis and take specific diagnostic and therapeutic measures to assess and reduce this risk.
P- Reviewer: Bener A S- Editor: Song XX L- Editor: A E- Editor: Lu YJ