Abstract
The epidemiology of systemic vasculitides differs between Japan, Europe and North America. Takayasu’s arteritis occurs frequently in Japan, unlike giant cell arteritis. A collaborative international study comparing the epidemiology of anti-neutrophil cytoplasmic antibody (ANCA)-associated vasculitis between Japan and the United Kingdom (UK) demonstrated that microscopic polyangiitis and myeloperoxidase-ANCA were more common in Japan whereas granulomatosis with polyangiitis and pronase 3-ANCA were more common in the UK. These differences may be attributed to differences in latitude and genetic backgounds. These findings provide useful information on the aetiology and pathogenesis of primary systemic vasculitides in various geographical regions.
Similar content being viewed by others
Introduction
The incidence and clinical features of several types of vasculitides differ between Japan, Europe and North America, unlike those of rheumatoid arthritis, systemic lupus erythematosus, and other rheumatic diseases in these geographical regions [1, 2]. These vasculitides are more rare and heterogeneous in terms of clinical features, types of anti-neutrophil cytoplasmic antibody (ANCA) and response to treatment. Because geographical differences in the incidence of ANCA-associated vasculitis (AAV) have been demonstrated in Europe [3], we extended our research to determine the incidence, clinical phenotype and the associated genetic factors of vasculitides between Japan, Europe, and North America. In this review, we present a brief account of the results of these studies.
Takayasu’s arteritis (TAK) and giant cell arteritis (GCA)
TAK and GCA are two types of vasculitis characterized by inflammation of the large vessels.
Histologically, both demonstrate granulomatous vasculitis with giant cells. Fewer patients with GCA have been reported in the Japanese literature than in the European and North American literatures. In contrast, more patients with TAK have been reported in Japan than in Europe or the USA [4]. The point prevalence of GCA in Japan was 690 patients in 1997 (95 % confidence interval [CI] 400–980) [5]. The prevalence of patients ≥50 years of age was 1.47 cases (95 % CI 0.86–2.10) per 10 million people in Japan compared with 200 and 60 cases per 10 million people in the USA and Spain, respectively [6, 7].
The reason for the low incidence of GCA in Japan remains unclear; however, genetic factors affecting the incidence of these diseases are unique and important. The HLA-DRB1*0401 and HLA-DRB1*0404 haplotypes are predominantly (60 %) detected in patients with GCA in America. These haplotypes were less frequently detected in 493 Japanese healthy controls (2.9 and 0.7 %, respectively) than in 60 American healthy controls (15.9 and 3.2 %, respectively) [5]. This explains why the incidence and/or prevalence of GCA is not high in Japan. Moreover, our study found no significant differences in the clinical features of GCA between Japan and other countries, although GCA cases are less common in Japan than in the USA or Europe [8].
TAK, which predominantly affects young females in Japan, affects the aortic arch (Type I), as determined by angiography. The incidence of HLA-B52 (56 %) and HLA-B39 (17 %) was significantly higher in patients with TAK than in healthy controls (25 and 6 %, respectively) in a Japanese study. However, several patients with TAK in India and other East Asian countries are reportedly middle-aged males who express HLA-B39 and exhibit abdominal aorta involvement (Type III).
ANCA-associated vasculitis (AAV)
Geographic factors: the latitude of Japan
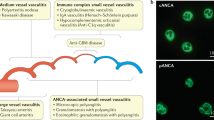
Japan is located between the latitudes of 26–45°N. Asahikawa city (43.5°N) on Hokkaido Island is close to the latitude of Lugo, Spain (42°N) [1]. On this island, there are more patients with microscopic polyangiitis (MPA); a higher number of patients with AAV are MPO-ANCA-positive than granulomatosis with polyangiitis (GPA)- or pronase 3 (PR3)-positive [1]. These data are compatible with the latitude theory of AAV [3] (Fig. 1).
On the other hand, it is interesting to note that a study from Beijing (39.5°N), China, demonstrated that 60.7 % (54/89) of patients with GPA were MPO-ANCA-positive and 38.2 % (34/89) were PR3-ANCA-positive. Patients with MPO-ANCA had multiorgan involvement with higher serum creatinine levels than PR3-ANCA-positive patients with GPA [9].
Differences in clinical phenotypes
Differences in renal involvement in GPA and MPA between patients in the UK and Japan were reported by Watts et al. [10]. Supporting data indicated that patients with localized GPA were more frequent than GPA patients with renal involvement in Japan, which was reported by Harabuchi et al. from Asahikawa Medical University and confirmed in our investigation [11]. Another report by certain otolaryngologists reached the same conclusion [12]. Moreover, two studies demonstrated renal involvement in 12–40 % of 21 patients with GPA [13, 14]. In another hospital-based, nationwide, retrospective study conducted in Japan from 1988 to 1998 by the Japanese Ministry of Health, Labour and Welfare, renal involvement was diagnosed in 39–63 % of 172 patients. In two studies by Gross et al. in Germany and Hoffman et al. in the USA, renal involvement was diagnosed in 77 % of 155 patients and 77 % of 70 patients with GPA, respectively [15, 16].
Genetic factors
A genetic analysis of patients with MPA was initiated in 1997 by the Research Committee of Intractable Vasculitis of the Japanese Ministry of Health and Welfare (Chief Investigator Prof. Hiroshi Hashimoto). A significant association between HLA-DRB1*0901 and MPA (P = 0.037; odds ratio [OR] 2.44; 95 % CI 1.33–4.46) as well as MPO-ANCA positivity (P = 0.014; OR 2.44; 95 % CI 1.41–4.22) was demonstrated by Tsuchiya et al. [17, 18]. Another report published in 1996 demonstrated an association between HLA-DR9 in 62.5 % patients and cANCA-positive GPA (10/16) compared with 26 % in healthy controls (P < 0.05) [19]. The decreased activation potential of natural killer cells and/or T cells associated with killer cell immunoglobulin-like receptor or HLA genotypes was demonstrated in patients with MPA, thus suggesting that these patients may have insufficient resistance to infections. An autoreactive T-cell response to the MPO fragments was detected in addition to the distinct epitopes of MPO fragments recognized by HLA-DR-restricted CD4 + T cells [20].
The Miyazaki-UK Study: a population-based, prospective study
The epidemiological manifestations of AAV differ between geographical regions [3]. However, there are no prospective studies comparing the incidence of AAV between Japan and Europe over the same time period using similar case definitions [10, 21]. The incidence of AAV in Miyazaki Prefecture, Japan, and Norfolk, UK, between 2005 and 2009, was prospectively determined using a population-based method. Patients with AAV were defined and classified according to the European Medicines Agency algorithm. The number of cases of AAV in Japan and the UK was 86 and 50, respectively, and the average annual incidence over the 5-year period was 22.6 per million people (95 % CI 19.1–26.2) and 21.8 per million people (95 % CI 12.6–30.9) in Japan and the UK, respectively. The average patient age was higher in Japan than the UK (mean [median]) 69.7 [72] vs 60.5 [61] years]. MPA was the predominant subtype in Japan (83 %), whereas GPA was more frequent in the UK (66 %). Regarding the pattern of ANCA positivity, >80 % patients in Japan were pANCA- and/or MPO-positive, whereas two-thirds of patients in the UK were cANCA- and/or PR3-positive. Renal involvement in patients with MPA was common in both countries but it was significantly less common in GPA patients in Japan than in GPA patients in the UK. There was no major difference in the incidence of AAV between Japan and the UK, but this prospective study found that MPA and MPO-ANCA were more common in Japan whereas GPA and PR3-ANCA were more common in the UK [21].
References
Kobayashi S, Fujimoto S, Takahashi K, Suzuki K. Anti-neutrophil cytoplasmic antibody-associated vasculitis, large vessel vasculitis and Kawasaki disease in Japan. Kidney Blood Press Res. 2010;33:442–55.
Watts RA, Lane SE, Bentham G, Scott DG. Epidemiology of systemic vasculitis: a ten-year study in the United Kingdom. Arthritis Rheum. 2000;43:414–9.
Watts RA, Gonzalez-Gay MA, Lane SE, Garcia-Porrua C, Bentham G, Scott DG. Geoepidemilogy of systemic vasculitis: comparison of the incidence in two regions of Europe. Ann Rheum Dis. 2001;60:170–2.
Numano F. Differences in clinical presentation and outcome in different countries for Takayasu’s arteritis. Curr Opin Rheumatol. 1997;9:12–5.
Kobayashi S, Yano T, Matsumoto Y, Numano F, Nakajima N, Yasuda K, Yutani C, Nakayama T, Tamakoshi A, Kawamura T, Ohno Y, Inaba Y, Hashimoto H. Clinical and epidemiologic analysis of giant cell (temporal) arteritis from a nationwide survey in 1998 in Japan: the first government-supported nationwide survey. Arthritis Rheum. 2003;49:594–8.
Lawrence RC, Helmick CG, Arnett FC, Deyo RA, Felson DT, Giannini EH, Heyse SP, Hirsch R, Hochberg MC, Hunder GG, Liang MH, Pillemer SR, Steen VD, Wolfe F. Estimates of the prevalence of arthritis and selected musculoskeletal disorders in the United States. Arthritis Rheum. 1998;41:778–99.
Gonzalez-Gay MA, Alonso MD, Aguero JJ, Bal M, Fernandez-Camblor B, Sanchez-Andrade A. Temporal arteritis in a northwestern area of Spain: study of 57 biopsy proven patients. J Rheumatol. 1992;19:277–80.
Kobayashi S, Yano T, Inaba Y, Hashimoto H, Matsumoto Y, Tamakoshi A, Kawamura T, Ohno Y. Ocular involvement of Japanese patients with giant cell arteritis from the first nation-wide survey. Arthritis Rheum. 2003;49:867–8.
Chen M, Yu F, Zhang Y, Zou WZ, Zhao MH, Wang HY. Characteristics of Chinese patients with wegener’s granulomatosis with anti-myeloperoxidase. Kidney Int. 2005;68:2225–9.
Watts RA, Scott DG, Jayne DR, Ito-Ihara T, Muso E, Fujimoto S, Harabuchi Y, Kobayashi S, Suzuki K, Hashimoto H, Watts RA, Scott DGI, Jayne DRW, et al. Renal vasculitis in Japan and the UK-are there differences in epidemiology and clinical phenotype? Nephrolol Dial Transplant. 2008;23:3928–31.
Kishibe K, Ueda S, Ishi H, Takahara K, Kunibe I, Katada A, Hayashi T, Harabuchi Y. Clinical manifestation of patients with Wegener’s granulomatosis in Asahikawa, Hokkaido. Oto-Rhino Laringol. 2009;112:396 (in Japanese).
Tsuzuki K, Fukazawa K, Takebayashi H, Hashimoto K, Sakagami M. Difficulty of diagnosing Wegener's granulomatosis in the head and neck region. Auris Nasus Larynx. 2009;36(1):64–70.
Ishida Y, Katada A, Kishibe K, Imada M, Hayashi T, Nonaka S, et al. Wegener’s granulomatosis with otolaryngological symptoms. Practica Oto-Rhino-Laryngologica. 2004;97:997–1005.
Takagi D, Nakamaru Y, Maguchi S, Furuta Y, Fukuda S. Otologic manifestations of Wegener’s granulomatosis. Laryngoscope. 2002;112:1684–90.
Reinhold-Keller E, Beuge N, Latza U, de Groot K, Rudert H, Nölle B, Heller M, Gross WL. An interdisciplinary approach to the care of patients with Wegener’s granulomatosis: long-term outcome in 155 patients. Arthritis Rheum. 2000;43:1021–32.
Hoffman GS, Kerr GS, Leavbitt RY, Hallahan CW, Lebovics RS, Travis W, et al. Wegener granulomatosis: an analysis of 158 patients. Ann Intern Med. 1992;116:488–98.
Tsuchiya N, Kobayashi S, Kawasaki A, Kyogoku C, Arimura Y, Yoshida M, Tokunaga K, Hashimoto H. Genetic background of Japanese patients with antineutrophil cytoplasmic antibody-associated vasculitis: association of HLA-DRB1*0901 with microscopic polyangiitis. J Rheumatol. 2003;30:1534–40.
Tsuchiya N, Kobayashi S, Hashimoto H, Ozaki S, Tokunaga K. Association of HLA-DRB1*0901-DQB1*0303 haplotype with microscopic polyangiitis in Japanese. Genes Immun. 2006;7:81–4.
Nakamaru Y, Maguchi S, Takizawa M, Fukuda S, Inuyama Y. The association between human leukocyte antigens (HLA) and cytoplasmic-antineutrophil cytoplasmic antibody (cANCA)-positive Wegener’s granulomatosis in a Japanese population. Rhinology. 1996;34:163–5.
Seta N, Kobayashi S, Hashimoto H, Kuwana M. Characterization of autoreactive T-cell clones to myeloperoxidase in patients with microscopic polyangiitis and healthy individuals. Clin Exp Rheumatol. 2009;27:826–9.
Fujimoto S, Watts RA, Kobayashi S, Suzuki K, Jayne DR, Scott DG, Hashimoto H, Nunoi H. Comparison of the epidemiology of anti-neutrophil cytoplasmic antibody-associated vasculitis between Japan and the U.K. Rheumatology (Oxford). 2011;50:1916–20.
Tougan T, Onda H, Okuzaki D, Kobayashi S, Hashimoto H, Nojima H. Focused microarray analysis of peripheral mononuclear blood cells from Churg−Strauss syndrome patients. DNA Res. 2008;15:103–14.
Kobayashi S, Ito A, Okuzaki D, Onda H, Yabuta N, Nagamori I, Suzuki K, Hashimoto H, Nojima H. Expression profiling of PBMC-based diagnostic gene markers isolated from vasculitis patients. DNA Res. 2008;15:253–65.
Acknowledgments
The work of the authors (SK and SF) discussed in this study was supported by a Grant-in-Aid from the Ministry of Health, Labour and Welfare of Japan.
Conflict of interest
The authors have declared that no conflict of interest exists.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Kobayashi, S., Fujimoto, S. Epidemiology of vasculitides: differences between Japan, Europe and North America. Clin Exp Nephrol 17, 611–614 (2013). https://doi.org/10.1007/s10157-013-0813-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-013-0813-9