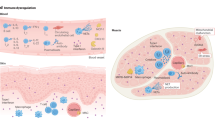
Abstract
Juvenile inflammatory myopathies represent a heterogeneous group of rare and potentially fatal disorders of unknown aetiology, characterised by inflammation and proximal and symmetric muscle weakness. Beyond many similarities, specific clinical, laboratoristic and histopathologic features underlie different subsets with distinguishing demographic, prognostic and therapeutic peculiarities. Over time, several forms of inflammatory idiopathic myopathies have been described, including macrophagic myofascitis, immune-mediated necrozing myopathy and the spectrum of amyopathic dermatomyositis that include hypomyopathic dermatomyositis, inclusion body myositis and cancer-associated myositis occurring almost exclusively in adults. However, juvenile dermatomyositis is the most frequent in childhood, whereas polymyositis is relatively more frequent in adults. The aetiology is nowadays widely unclear; however, current theories contemplate a combination of environmental triggers, immune dysfunction and specific tissue responses involving muscle, skin and small vessels endothelium in genetically susceptible individuals. Myositis-specific autoantibodies, found almost exclusively in patients with myositis and myositis-associated autoantibodies, detectable both among patients with myositis and in subjects suffering from other autoimmune diseases, have an important clinical role because of their relation to specific clinical features, response to therapy and prognosis. The gold standard treatment for juvenile dermatomyositis is represented by corticosteroids, along with adjunctive steroid-sparing immunosuppressive therapies, which are used to counteract disease activity, prevent mortality, and reduce long-term disability. Further treatment approach such as biologic agents and autologous stem cell transplantation are emerging during the last years, in particular in patients difficult to treat and with poor prognosis. Therefore, a highly medical specialised approach is required for diagnosis and management of these conditions. This review comprehensively examines juvenile inflammatory myopathies focusing on clinical and laboratory classifications as well as on the current treatment approaches, referring in particular on biologic agents and latest therapeutic opportunities.




Similar content being viewed by others
References
Feldman BM, Rider LG, Reed AM, Pachman LM (2008) Juvenile dermatomyositis and other idiopathic inflammatory myopathies of childhood. Lancet 371:2201–2212
Robinson AB, Reed AM (2011) Clinical features, pathogenesis and treatment of juvenile and adult dermatomyositis. Nat Rev Rheumatol 7:664–675
Bohan A, Peter JB (1975) Polymyositis and dermatomyositis (second of two parts). N Engl J Med 292:403–407
Bohan A, Peter JB (1975) Polymyositis and dermatomyositis (first of two parts). N Engl J Med 292:344–347
Brown VE, Pilkington CA, Feldman BM, Davidson JE, Network for Juvenile Dermatomyositis, Paediatric Rheumatology European Society (PReS) (2006) An international consensus survey of the diagnostic criteria for juvenile dermatomyositis (JDM). Rheumatology (Oxford) 45:990–993
Rider LG, Katz JD, Jones OY (2013) Developments in the classification and treatment of the juvenile idiopathic inflammatory myopathies. Rheum Dis Clin N Am 39:877–904
Stringer E, Singh-Grewal D, Feldman BM (2008) Predicting the course of juvenile dermatomyositis: significance of early clinical and laboratory features. Arthritis Rheum 58:3585–3592, Erratum in: Arthritis Rheum. 58:3950
Sultan SM, Ioannou Y, Moss K, Isenberg DA (2002) Outcome in patients with idiopathic inflammatory myositis: morbidity and mortality. Rheumatology (Oxford) 41:22–26
Ravelli A, Trail L, Ferrari C et al (2010) Long-term outcome and prognostic factors of juvenile dermatomyositis: a multinational, multicenter study of 490 patients. Arthritis Care Res 62:63–72
Bingham A, Mamyrova G, Rother KI et al (2008) Predictors of Acquired Lipodystrophy in Juvenile-Onset Dermatomyositis and a Gradient of Severity. Medicine (Baltimore) 87:70–86
Crowe WE, Bove KE, Levinson JE, Hilton PK (1982) Clinical and pathogenetic implications of histopathology in childhood polydermatomyositis. Arthritis Rheum 25:126–139
Dalakas MC, Hohlfeld R (2003) Polymyositis and dermatomyositis. Lancet 362:971–982
Harris-Love MO, Shrader JA, Koziol D et al (2009) Distribution and severity of weakness among patients with polymyositis, dermatomyositis and juvenile dermatomyositis. Rheumatology (Oxford) 48:134–139
Gerami P, Walling HW, Lewis J, Doughty L, Sontheimer RD (2007) (2007), A systematic review of juvenile-onset clinically amyopathic dermatomyositis. Br J Dermatol 157:637–644
Ibarra M, Chou P, Pachman LM (2011) Ovarian teratoma mimicking features of juvenile dermatomyositis in a child. Pediatrics 128:e1293–e1296
Morris P, Dare J (2010) Juvenile dermatomyositis as a paraneoplastic phenomenon: an update. J Pediatr Hematol Oncol 32:189–191
Rider LG, Shah M, Mamyrova G et al (2013) The myositis autoantibody phenotypes of the juvenile idiopathic inflammatory myopathies. Medicine (Baltimore) 92:223–243
Gunawardena H, Wedderburn LR, North J et al (2008) Clinical associations of autoantibodies to a p155/140 kDa doublet protein in juvenile dermatomyositis. Rheumatology (Oxford) 47:324–328
Trallero-Araguás E, Rodrigo-Pendás JÁ, Selva-O’Callaghan A et al (2012) Usefulness of anti-p155 autoantibody for diagnosing cancer-associated dermatomyositis: a systematic review and meta-analysis. Arthritis Rheum 64:523–532
Espada G, Maldonado Cocco JA, Fertig N, Oddis CV (2009) Clinical and serologic characterization of an Argentine pediatric myositis cohort: identification of a novel autoantibody (anti-MJ) to a 142-kDa protein. J Rheumatol 36:2547–2551
Gunawardena H, Wedderburn LR, Chinoy H et al (2009) Autoantibodies to a 140-kd protein in juvenile dermatomyositis are associated with calcinosis. Arthritis Rheum 60:1807–1814
Love LA, Leff RL, Fraser DD et al (1991) A new approach to the classification of idiopathic inflammatory myopathy: myositis-specific autoantibodies define useful homogeneous patient groups. Medicine (Baltimore) 70:360–374
Rouster-Stevens KA, Pachman LM (2008) Autoantibody to signal recognition particle in African American girls with juvenile polymyositis. J Rheumatol 35:927–929
Sakurai N, Nagai K, Tsutsumi H, Ichimiya S (2011) Anti-CADM-140 antibody-positive juvenile dermatomyositis with rapidly progressive interstitial lung disease and cardiac involvement. J Rheumatol 38:963–964
Fujimoto M, Hamaguchi Y, Kaji K et al (2012) Myositis-specific anti-155/140 autoantibodies target transcription intermediary factor 1 family proteins. Arthritis Rheum 64:513–522
Shah M, Mamyrova G, Targoff IN et al (2013) The clinical phenotypes of the juvenile idiopathic inflammatory myopathies. Medicine (Baltimore) 92:25–41
Wedderburn LR, McHugh NJ, Chinoy H et al (2007) HLA class II haplotype and autoantibody associations in children with juvenile dermatomyositis and juvenile dermatomyositis-scleroderma overlap. Rheumatology (Oxford) 46:1786–1791
Tansley S, Gunawardena H (2014) The evolving spectrum of polymyositis and dermatomyositis--moving towards clinicoserological syndromes: a critical review. Clin Rev Allergy Immunol 47:264–273
Venalis P, Lundberg IE (2013) Immune mechanisms in polymyositis and dermatomyositis and potential targets for therapy. Rheumatology (Oxford) 53:397–405
Wedderburn LR, Rider LG (2009) Juvenile dermatomyositis: new developments in pathogenesis, assessment and treatment. Best Pract Res Clin Rheumatol 23:665–678
Mamyrova G, O’Hanlon TP, Monroe JB et al (2006) Immunogenetic risk and protective factors for juvenile dermatomyositis in Caicasians. Arthritis Rheum 4:3979–3987
Chinoy H, Payne D, Poulton KV et al (2009) HLA-DPB1 associations differ between DRB1*03 positive anti-Jo-1 and anti-PM-Scl antibody positive idiopathic inflammatory myopathy. Rheumatology (Oxford) 48:1213–1217
Mastaglia FL (2007) Sporadic inclusion body myositis: variability in prevalence and phenotype and influence of the MHC. Acta Myol 28:66–71
Rider LG (2007) The heterogeneity of juvenile myositis. Autoimmun Rev 6:241–247
Chinoy H, Platt H, Lamb JA et al (2008) The protein tyrosine phosphatase N22 gene is associated with juvenile and adult idiopathic inflammatory myopathy independent of the HLA 8.1 haplotype in British Caucasian patients. Arthritis Rheum 58:3247–3254
O’Hanlon TP, Rider LG, Schiffenbauer A et al (2008) Immunoglobulin gene polymorphisms are susceptibility factors in clinical and autoantibody subgroups of the idiopathic inflammatory myopathies. Arthritis Rheum 58:3239–3246
Pachman LM, Liotta-Davis MR, Hong DK et al (2000) TNFalpha-308A allele in juvenile dermatomyositis: association with increased production of tumor necrosis factor alpha, disease duration, and pathologic calcifications. Arthritis Rheum 43:2368–2377
Pachman LM, Lipton R, Ramsey-Goldman R et al (2005) History of infection before the onset of juvenile dermatomyositis: results from the National Institute of Arthritis and Musculoskeletal and Skin Diseases Research Registry. Arthritis Rheum 53:166–172
Pachman LM, Litt DL, Rowley AH et al (1995) Lack of detection of enteroviral RNA or bacterial DNA in magnetic resonance imaging-directed muscle biopsies from twenty children with active untreated juvenile dermatomyositis. Arthritis Rheum 38:1513–1518
Mamyrova G, Rider LG, Haagenson L, Wong S, Brown KE (2005) Parvovirus B19 and onset of juvenile dermatomyositis. JAMA 294:2170–2171
Stringer E, Bohnsack J, Bowyer SL et al (2010) Treatment approaches to juvenile dermatomyositis (JDM) across North America: The Childhood Arthritis and Rheumatology Research Alliance (CARRA) JDM Treatment Survey. J Rheumatol 37:1953–1961
Hasija R, Pistorio A, Ravelli A et al (2011) Therapeutic approaches in the treatment of juvenile dermatomyositis in patients with recent-onset disease and in those experiencing disease flare: an international multicenter PRINTO study. Arthritis Rheum 63:3142–3152
Huber AM, Giannini EH, Bowyer SL et al (2010) Protocols for the initial treatment of moderately severe juvenile dermatomyositis: results of a Children’s Arthritis and Rheumatology Research Alliance Consensus Conference. Arthritis Care Res 62:219–225
Huber AM, Robinson AB, Reed AM et al (2012) Subcommittee of the Childhood Arthritis and Rheumatology Research Alliance Consensus treatments for moderate juvenile dermatomyositis: beyond the first two months. Results of the second Childhood Arthritis and Rheumatology Research Alliance consensus conference. Arthritis Care Res 64:546–553
Seshadri R, Feldman BM, Ilowite N, Cawkwell G, Pachman LM (2008) The role of aggressive corticosteroid therapy in patients with juvenile dermatomyositis: a propensity score analysis. Arthritis Rheum 59:989–995
Ramanan AV, Campbell-Webster N, Ota S et al (2005) The effectiveness of treating juvenile dermatomyositis with methotrexate and aggressively tapered corticosteroids. Arthritis Rheum 52:3570–3578
Ruperto N, Pistorio A, Oliveira S et al (2012) A randomized trial in new onset juvenile dermatomyositis: prednisone versus prednisone plus cyclosporine versus prednisone plus methotrexate. Arthritis Rheum 64:S1042–S1043 [Abstract]
Lam CG, Manlhiot C, Pullenayegum EM, Feldman BM (2011) Efficacy of intravenous Ig therapy in juvenile dermatomyositis. Ann Rheum Dis 70:2089–2094
Dagher R, Desjonqueres M, Duquesne A et al (2012) Mycophenolate mofetil in juvenile dermatomyositis: a case series. Rheumatol Int 32:711–716
Wilkes MR, Sereika SM, Fertig N, Lucas MR, Oddis CV (2005) Treatment of antisynthetase-associated interstitial lung disease with tacrolimus. Arthritis Rheum 52:2439–2446
Hassan J, van der Net JJ, van Royen-Kerkhof A (2008) Treatment of refractory juvenile dermatomyositis with tacrolimus. Clin Rheumatol 27:1469–1471
Riley P, Maillard SM, Wedderburn LR, Woo P, Murray KJ, Pilkington CA (2004) Intravenous cyclophosphamide pulse therapy in juvenile dermatomyositis A review of efficacy and safety. Rheumatology (Oxford) 43:491–496
Levine T (2012) Treating refractory dermatomyositis or polymyositis with adrenocorticotropic hormone gel: a retrospective case series. Drug Des Devel Ther 6:133–139, Erratum in: Drug Des Devel Ther. 6:163
Chiu YE, Co DO (2011) Juvenile dermatomyositis: immunopathogenesis, role of myositis-specific autoantibodies, and review of rituximab use. Pediatr Dermatol 28:357–367, Erratum in: Pediatr Dermatol. 28:627
Chung L, Genovese MC, Fiorentino DF (2007) A pilot trial of rituximab in the treatment of patients with dermatomyositis. Arch Dermatol 143:763–767
Oddis CV, Reed AM, Aggarwal R et al (2013) Rituximab in the treatment of refractory adult and juvenile dermatomyositis and adult polymyositis: a randomized, placebo-phase trial. Arthritis Rheum 65:314–324
Unger L, Kampf S, Lüthke K, Aringer M (2014) Rituximab therapy in patients with refractory dermatomyositis or polymyositis: differential effects in a real-life population. Rheumatology (Oxford) 53:1630–1638
Basnayake C, Cash K, Blumbergs P, Limaye V (2013) Use of rituximab in histologically confirmed idiopathic inflammatory myositis: a case series. Clin Rheumatol
Nalotto L, Iaccarino L, Zen M et al Rituximab in refractory idiopathic inflammatory myopathies and antisynthetase syndrome: personal experience and review of the literature. Immunol Res. 56:362–70
Muñoz-Beamud F, Isenberg DA (2013) Rituximab as an effective alternative therapy in refractory idiopathic inflammatory myopathies. Clin Exp Rheumatol 31:896–903
Aggarwal R, Bandos A, Reed AM et al (2014) Predictors of clinical improvement in rituximab-treated refractory adult and juvenile dermatomyositis and adult polymyositis. Arthritis Rheumatol 66:740–749
Molloy ES, Calabrese LH (2012) Progressive multifocal leukoencephalopathy associated with immunosuppressive therapy in rheumatic diseases: evolving role of biologic therapies. Arthritis Rheum 64:3043–3051
Riley P, McCann LJ, Maillard SM, Woo P, Murray KJ, Pilkington CA (2008) Effectiveness of infliximab in the treatment of refractory juvenile dermatomyositis with calcinosis. Rheumatology (Oxford) 47:877–880
Hengstman GJ, van den Hoogen FH, Barrera P et al (2003) Successful treatment of dermatomyositis and polymyositis with anti-tumor-necrosis-factor-alpha: preliminary observations. Eur Neurol 50:10–15
Anandacoomarasamy A, Howe G, Manolios N (2005) Advanced refractory polymyositis responding to infliximab. Rheumatology (Oxford) 44:562–563
Efthimiou P, Schwartzman S, Kagen LJ (2006) Possible role for tumour necrosis factor inhibitors in the treatment of resistant dermatomyositis and polymyositis: a retrospective study of eight patients. Ann Rheum Dis 65:1233–1236
Chen D, Wang XB, Zhou Y, Zhu XC (2013) Efficacy of infliximab in the treatment for dermatomyositis with acute interstitial pneumonia: a study of fourteen cases and literature review. Rheumatol Int 33:2455–2458
Muscle Study Group (2011) A randomized, pilot trial of etanercept in dermatomyositis. Ann Neurol 70:427–436
Coyle K, Pokrovnichka A, French K et al (2008) A Randomized, Double-Blind Placebo-Controlled Trial of Infliximab in Patients with Polymyositis and Dermatomyositis. Arthritis Rheum 58:S923–S924
Hengstman GJ, De Bleecker JL, Feist E et al (2008) Open-label trial of anti-TNF-alpha in dermato- and polymyositis treated concomitantly with methotrexate. Eur Neurol 59:159–163
Dastmalchi M, Grundtman C, Alexanderson H et al (2008) A high incidence of disease flares in an open pilot study of infliximab in patients with refractory inflammatory myopathies. Ann Rheum Dis 67:1670–1677
Rouster-Stevens KA, Ferguson L, Morgan G, Huang CC, Pachman LM (2014) Pilot study of etanercept in patients with refractory juvenile dermatomyositis. Arthritis Care Res 66:783–787
Iannone F, Scioscia C, Falappone PC, Covelli M, Lapadula G (2006) Use of etanercept in the treatment of dermatomyositis: a case series. J Rheumatol 33:1802–1804
Klein R, Rosenbach M, Kim EJ, Kim B, Werth VP, Dunham J (2010) Tumor necrosis factor inhibitor-associated dermatomyositis. Arch Dermatol 146:780–784
Brunasso AM, Aberer W, Massone C (2014) New onset of dermatomyositis/polymyositis during anti-TNF-α therapies: a systematic literature review. Sci World J 2014:179180
Liu SW, Velez NF, Lam C et al (2013) Dermatomyositis induced by anti-tumor necrosis factor in a patient with juvenile idiopathic arthritis. JAMA Dermatol 149:1204–1208
Zong M, Dorph C, Dastmalchi M et al (2013) Anakinra treatment in patients with refractory inflammatory myopathies and possible predictive response biomarkers: a mechanistic study with 12 months follow-up. Ann Rheum Dis 73:913–920
Kosmidis ML, Alexopoulos H, Tzioufas AG, Dalakas MC (2013) The effect of anakinra, an IL1 receptor antagonist, in patients with sporadic inclusion body myositis (sIBM): a small pilot study. J Neurol Sci 334:123–125
Okiyama N, Sugihara T, Iwakura Y, Yokozeki H, Miyasaka N, Kohsaka H (2009) Therapeutic effects of interleukin-6 blockade in a murine model of polymyositis that does not require interleukin-17A. Arthritis Rheum 60:2505–2512
Narazaki M, Hagihara K, Shima Y, Ogata A, Kishimoto T, Tanaka T (2011) Therapeutic effect of tocilizumab on two patients with polymyositis. Rheumatology (Oxford) 50:1344–1346
Kerola AM, Kauppi MJ (2014), Abatacept as a successful therapy for myositis-a case-based review. Clin Rheumatol
Musuruana JL, Cavallasca JA (2011) Abatacept for treatment of refractory polymyositis. Joint Bone Spine 78:431–432
Arabshahi B, Silverman RA, Jones OY, Rider LG (2012) Abatacept and sodium thiosulfate for treatment of recalcitrant juvenile dermatomyositis complicated by ulceration and calcinosis. J Pediatr 160:520–522
Dalakas MC, Rakocevic G, Schmidt J et al (2009) Effect of Alemtuzumab (CAMPATH 1-H) in patients with inclusion-body myositis. Brain 132:1536–1544
Thompson B, Corris P, Miller JA, Cooper RG, Halsey JP, Isaacs JD (2008) Alemtuzumab (Campath-1H) for treatment of refractory polymyositis. J Rheumatol 35:2080–2082
Cooles FA, Jackson GH, Menon G, Isaacs JD (2011) Epstein-Barr virus-driven lymphoproliferative disorder post-CAMPATH-1H (alemtuzumab) in refractory polymyositis. Rheumatology (Oxford) 50:810–812
Henes JC, Heinzelmann F, Wacker A et al (2009) Antisignal recognition particle-positive polymyositis successfully treated with myeloablative autologous stem cell transplantation. Ann Rheum Dis 68:447–448
Higgs BW, Zhu W, Morehouse C et al (2014) A phase 1b clinical trial evaluating sifalimumab, an anti-IFN-α monoclonal antibody, shows target neutralisation of a type I IFN signature in blood of dermatomyositis and polymyositis patients. Ann Rheum Dis 73:256–262
Guo X, Higgs BW, Rebelatto M et al (2014) Suppression of soluble T cell-associated proteins by an anti-interferon-α monoclonal antibody in adult patients with dermatomyositis or polymyositis. Rheumatology (Oxford) 53:686–695
Holzer U, van Royen-Kerkhof A, van der Torre P et al (2010) Successful autologous stem cell transplantation in two patients with juvenile dermatomyositis. Scand J Rheumatol 39:88–92
Baron F, Ribbens C, Kaye O, Fillet G, Malaise M, Beguin Y (2000) Effective treatment of Jo-1-associated polymyositis with T-cell-depleted autologous peripheral blood stem cell transplantation. Br J Haematol 110:339–342
Oryoji K, Himeji D, Nagafuji K et al (2005) Successful treatment of rapidly progressive interstitial pneumonia with autologous peripheral blood stem cell transplantation in a patient with dermatomyositis. Clin Rheumatol 24:637–640
Storek J, LeClercq SA, Aaron SL (2013) Lack of sustained response of advanced dermatomyositis to autologous haematopoietic cell transplantation. Scand J Rheumatol 42:421–422
Bingham S, Griffiths B, McGonagle D, Snowden JA, Morgan G, Emery P (2001) Autologous stem cell transplantation for rapidly progressive Jo-1-positive polymyositis with long-term follow-up. Br J Haematol 113:840–841
Walling HW, Gerami P, Sontheimer RD (2010) Juvenile-onset clinically amyopathic dermatomyositis: an overview of recent progress in diagnosis and management. Paediatr Drugs 12:23–34
Chander S, Gordon P (2012) Soft tissue and subcutaneous calcification in connective tissue diseases. Curr Opin Rheumatol 24:158–164
Pagnini L, Simonini G, Giani T et al (2014) Sodium thiosulfate for the treatment of calcinosis secondary to juvenile dermatomyositis. Clin Exp Rheumatol 32:408–409
Author information
Authors and Affiliations
Corresponding author
Additional information
Rolando Cimaz and Luca Cantarini contributed equally to this work.
Rights and permissions
About this article
Cite this article
Pagnini, I., Vitale, A., Selmi, C. et al. Idiopathic Inflammatory Myopathies: an Update on Classification and Treatment with Special Focus on Juvenile Forms. Clinic Rev Allerg Immunol 52, 34–44 (2017). https://doi.org/10.1007/s12016-015-8512-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12016-015-8512-9