Abstract
Background and Objectives
Systemic lupus erythematosus (SLE) is a multisystem complex autoimmune disease that often mimics symptoms of other illnesses, which complicates the ability of healthcare providers to make the diagnosis. The objective of this study was to assess clinical outcomes, resource utilization, and costs between patients with earlier versus later SLE diagnosis.
Methods
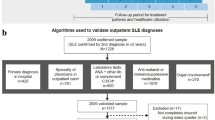
Patients aged 18–64 years were identified from a large US commercial claims database between January 2000 and June 2010. Confirmed SLE diagnosis with a claims-based algorithm required either three or more claims for a visit to a rheumatologist on separate dates with an SLE diagnosis (International Classification of Diseases [ICD-9] code 710.0x), two or more claims for visits to a rheumatologist at least 60 days apart with SLE diagnoses, or two or more claims for visits to rheumatologist less than 60 days apart with SLE diagnoses with at least one dispensing for a typical SLE medication. SLE probable onset date was identified during the 12-month baseline period by the second claim for antinuclear antibody tests or prodromal symptoms of SLE. Patients were stratified into early or late diagnosis groups based on time between probable SLE onset and diagnosis (<6 months or ≥6 months, respectively). Each patient observation period began on the date of the first medical claim, with a diagnosis code for SLE that satisfied the inclusion criteria, and ended on the earliest date between health plan disenrollment and 30 June 2010. Patients in each group were propensity-score matched on age, gender, diagnosis year, region, health plan type, and comorbidities. Flare rates and resource utilization were compared post-diagnosis between groups using rate ratios. All-cause and SLE-related costs (adjusted to 2010 US dollars) per patient per month (PPPM) were calculated.
Results
There were 4,166 matched patients per group. Post-SLE diagnosis, the early diagnosis group had lower rates of mild (rate ratio [RR] 0.95; 95 % CI 0.93–0.96), moderate (RR 0.96; 95 % CI 0.94–0.99), and severe (RR 0.87; 95 % CI 0.82–0.93) flares compared with the late diagnosis group. The rates of hospitalizations (RR 0.80; 95 % CI 0.75–0.85) were lower for the early diagnosis group than the late diagnosis group. Compared with late diagnosis patients, mean all-cause inpatient costs PPPM were lower for the early diagnosis patients (US$406 vs. US$486; p = 0.016). Corresponding SLE-related hospitalization costs were also lower for early compared with late diagnosis patients (US$71 vs. US$95; p = 0.013). Results were consistent for other resource use and cost categories.
Conclusions
Patients diagnosed with SLE sooner may experience lower flare rates, less healthcare utilization, and lower costs from a commercially insured population perspective. This finding needs to be further explored within the context of background SLE disease activity.


Similar content being viewed by others
References
Guidelines for referral and management of systemic lupus erythematosus in adults. American College of Rheumatology Ad Hoc Committee on Systemic Lupus Erythematosus Guidelines. Arthritis Rheum. 1999;42(9):1785–96.
How is lupus diagnoses. Lupus Foundation of America, Inc. http://www.lupus.org/answers/entry/diagnosing-lupus. Accessed 17 Dec 2013.
Doria A, Zen M, Canova M, Bettio S, Bassi N, Nalotto L, et al. SLE diagnosis and treatment: when early is early. Autoimmun Rev. 2010;10(1):55–60 Epub 2010 Sep 8.
Wallace DJ, Podell T, Weiner J, Klinenberg JR, Forouzesh S, Dubois EL. Systemic lupus erythematosus: survival patterns. Experience with 609 patients. JAMA. 1981;245:934–8.
Cervera R, Khamashta MA, Font J, et al. Cervera R, Khamashta MA, Font J, Sebastiani GD, Gil A, Lavilla P, et al. Clinical and immunologic patterns of disease expression in a cohort of 1,000 patients. The European Working Party on Systemic Lupus Erythematosus. Medicine. 1993;72:113–24.
Ozbek S, Sert M, Paydas S, Soy M. Delay in the diagnosis of SLE: the importance of arthritis/arthralgia as the initial symptom. Acta Med Okayama. 2003;57(4):187–90.
Li T, Carls GS, Panopalis P, et al. Long-term medical costs and resource utilization in systemic lupus erythematosus and lupus nephritis: a five-year analysis of a large Medicaid population. Arthritis Rheum. 2009;61:755–63.
Panopalis P, Yazdany J, Gillis JZ, et al. Health care costs and costs associated with changes in work productivity among persons with systemic lupus erythematosus. Arthritis Rheum. 2008;59:1788–95.
Carls G, Li T, Panopalis P, et al. Direct and indirect costs to employers of patients with systemic lupus erythematosus with and without nephritis. J Occup Environ Med. 2009;51:66–79.
Yelin E, Trupin L, Katz P, et al. Impact of health maintenance organizations and fee-for-service on health care utilization among people with systemic lupus erythematosus. Arthritis Rheum. 2007;57:508–15.
Pelletier EM, Ogale S, Yu E, et al. Economic outcomes in patients diagnosed with systemic lupus erythematosus with versus without nephritis: results from an analysis of data from a US claims database. Clin Ther. 2009;31:2653–64.
Furst DE, Clarke A, Fernandes AW, et al. Resource utilization and direct medical costs in adult systemic lupus erythematosus patients from a commercially insured population. Lupus. 2013;22(3):268–78.
Chibnik LB, Massarotti EM, Costenbader KH. Identification and validation of lupus nephritis cases using administrative data. Lupus. 2010;19(6):741–3.
Hahn B, Singh R. Animal models of SLE. In: Wallace DJ, Hahn BH, editors. Dubois’ Lupus Erythematosus 7th ed. 2007; p. 299–355.
Faurschou M, Starklint H, Halberg P, Jacobsen S. Prognostic factors in lupus nephritis: diagnostic and therapeutic delay increases the risk of terminal renal failure. J Rheumatol. 2006;33(8):1563–9.
Garris CP, Jhingran PM, Engel-Nitz NM, et al. Assessing systemic lupus erythematosus disease severity and disease flares: development of a claims-based algorithm. Arthritis Rheum. 2010;62 Suppl:757.
Quan H, Sundararajan V, Halfon P, et al. Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care. 2005;43:1130–9.
Mayo Clinic. Lupus complications. http://www.mayoclinic.com/health/lupus/DS00115/DSECTION=complications. Accessed 17 Dec 2013.
Alliance for Lupus Research. Cardiovascular disease and lupus. http://www.lupusresearch.org/research/acr/cardiovascular.html. Accessed 17 Dec 2013.
Bhatt SP, Handa R, Gulati GS, et al. Peripheral vascular disease in systemic lupus erythematosus. Lupus. 2007;16:720–3.
Keane MP, Lynch JP 3rd. Pleuropulmonary manifestations of systemic lupus erythematosus. Thorax. 2000;55:159–66.
Sen D, Keen RW. Osteoporosis in systemic lupus erythematosus: prevention and treatment. Lupus. 2001;10:227–32.
Appenzeller S, Pallone AT, Natalin RA, Costallat LT. Prevalence of thyroid dysfunction in systemic lupus erythematosus. J Clin Rheumatol. 2009;15:117–9.
Pyne D, Isenberg DA. Autoimmune thyroid disease in systemic lupus erythematosus. Ann Rheum Dis. 2002;61:70–2.
Bruce IN, Urowitz MB, Gladman DD, Hallett DC. Natural history of hypercholesterolemia in systemic lupus erythematosus. J Rheumatol. 1999;26:2137–43.
Doria A, et al. Long-term prognosis and causes of death in systemic lupus erythematosus. Am J Med. 2006;119:700–6.
Esdaile JM, Joseph L, MacKenzie T, Kashgarian M, Hayslett JP. The benefit of early treatment with immunosuppressive agents in lupus nephritis. J Rhematol. 1994;21(11):2046–51.
Doria A, Rinaldi S, Ermani M, et al. Health-related quality of life in Italian patients with systemic lupus erythematosus. II: Role of clinical, immunological and psychological determinants. Rheumatology. 2004;43:1580–6.
Acknowledgments
This study was funded by GlaxoSmithKline (GSK), Collegeville, PA, USA. The funding from GSK was not contingent upon the study results. GSK and Human Genome Sciences (HGS) participated in the study design, results interpretation, and manuscript preparation, as reflected in the authorship by GSK and HGS employees, Alan Oglesby and Gregory Dennis, respectively. A human monoclonal antibody, belimumab (Benlysta), was developed by GSK and HGS, and was recently approved for SLE treatment in the US, Canada, and Europe. Caroline Korves, François Laliberté, Sapna Rao, and Mei Sheng Duh are employees of Analysis Group, Inc., which received a research grant from GSK for this study. Ellison Dial Suthoff and Robert Wei were employees of Analysis Group, Inc. at the time this study was conducted.
Parts of the manuscript were presented as posters at the Annual European League Against Rheumatism (EULAR) Congress, Berlin, Germany, 6–9 June 2012, and at the International Society for Pharmacoeconomics and Outcomes Research (ISPOR) 17th Annual International Meeting, Washington, DC, USA, 2–6 June 2012.
Author Contributions
Study concept and design and data interpretation were primarily the work of Alan Oglesby, Mei Sheng Duh, François Laliberté, and Gregory Dennis, with assistance from the other authors. Caroline Korves, Sapna Rao, Ellison Dial Suthoff, and Robert Wei performed the data collection. Writing of the manuscript was shared by Caroline Korves, François Laliberté, and Mei Sheng Duh. Revision of the manuscript was shared by Alan Oglesby, Mei Sheng Duh, and Gregory Dennis.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendix
Appendix
Systemic lupus erythematosus severity (as defined by Garris et al. [16])a
Moderate | Moderate Rx or moderate medical condition |
|---|---|
Rx | Oral corticosteroid dose ≥7.5 mg/day to <60 mg/day |
Immunosuppressive agent (excluding cyclophosphamide) | |
Medical condition | Cardiorespiratory: myocarditis, pericarditis, pleurisy/pleural effusion, vasculitis (excluding aortitis) |
Constitutional: hepatitis (non-viral) | |
Gastrointestinal: acute pancreatitis, lupus enterititis/colitis | |
Hematology: hemolytic anemia | |
Musculoskeletal: ischemic necrosis of bone | |
Neuropsychiatric: demyelinating syndrome/acute inflammatory demyelinating polyradiculoneuropathy, mononeuropathy/polyneuropathy, myelopathy, pseudotumor cerebri, seizure |
High | Intensive Rx or severe medical condition |
|---|---|
Rx | Oral corticosteroid dose ≥60 mg/day |
Cyclophosphamide | |
Rituximab | |
Medical condition | Cardiorespiratory: aortitis, arterial/ venous thrombosis, cardiac tamponade, pulmonary hemorrhage, stroke/transient ischemic attack |
Gastrointestinal: intestinal pseudo-obstruction | |
Neuropsychiatric: acute confusional state/psychosis, aseptic meningitis, cranial neuropathy | |
Ophthalmic: optic neuritis | |
Renal: end stage renal disease |
Rights and permissions
About this article
Cite this article
Oglesby, A., Korves, C., Laliberté, F. et al. Impact of Early Versus Late Systemic Lupus Erythematosus Diagnosis on Clinical and Economic Outcomes. Appl Health Econ Health Policy 12, 179–190 (2014). https://doi.org/10.1007/s40258-014-0085-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40258-014-0085-x